Shocking Truth About Cesarean Scar Pregnancy You Must Know
If you’ve had a cesarean section in the past and you’re now pregnant again, there’s something your doctor will look for very carefully in the early weeks — something called a Cesarean Scar Pregnancy, or CSP. It’s rare, it’s serious, but most importantly, when caught early, it’s very treatable.
At Vasundhara Hospital, our gynecology team encounters questions about this condition regularly — especially from women who are pregnant after a previous C-section and are anxious about what to expect. This article is our attempt to answer those questions honestly, clearly, and with the warmth that every woman navigating a complex pregnancy deserves.
1. What Exactly is a Cesarean Scar Pregnancy?
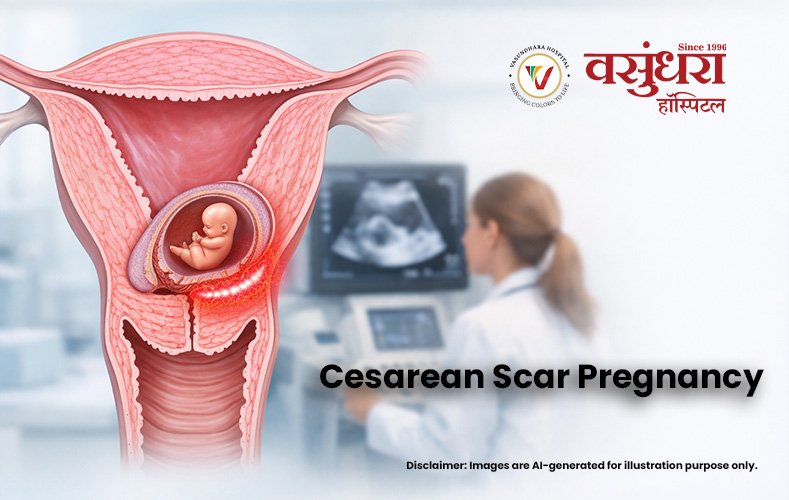
When a woman undergoes a cesarean delivery, a horizontal incision is made on the lower segment of the uterus. Over time, this heals into a scar. But like any scar in the body, this tissue isn’t quite the same as the original. It can be thinner, less vascular, and structurally different from the surrounding uterine wall.
A Cesarean Scar Pregnancy occurs when a fertilized egg, instead of traveling to the uterine cavity and implanting there, ends up implanting directly into this scar tissue. The embryo burrows into the fibrous scar, which cannot support a growing pregnancy the way normal uterine muscle can.
CSP is the implantation of a gestational sac within the myometrium at the site of a previous uterine scar — most often following a cesarean section. It accounts for less than 1% of all ectopic pregnancies but carries one of the highest complication rates among them.
2. Why Does It Happen?
The honest answer is — we don’t always know why. The fertilized egg makes its journey down the fallopian tube and into the uterus, and in most pregnancies, it finds its way to the uterine lining without trouble. But in women who have a uterine scar, there is a theory that tiny microscopic tracts or channels can form within the scar tissue during healing. These tracts may create a path that guides — or traps — the early embryo before it reaches the uterine cavity.
There may also be a role played by abnormal uterine contractions and altered blood flow patterns near scar tissue that cause the embryo to “stick” in the wrong place.
Known risk factors
- Previous cesarean section — the more you’ve had, the higher the risk
- Prior uterine surgeries such as myomectomy or curettage
- In vitro fertilization (IVF), which may place the embryo closer to the scar
- Short interval between the previous C-section and the current pregnancy
- Asherman’s syndrome or intrauterine adhesions
- Poorly healed or infected cesarean wound
3. How Common is it?
CSP is rare — but with the global rise in cesarean delivery rates, it’s becoming less rare than it once was. Two to three decades ago, it was almost a case report. Today, more and more gynecologists are encountering it in clinical practice.
1:1800
Estimated incidence among all pregnancies
6%
Of ectopic pregnancies in women with prior C-section
~45%
Rise in reported cases linked to increasing C-section rates globally
6–10 wks
Gestational age when most cases are discovered
India, in particular, has seen a significant rise in cesarean deliveries in recent years — both in government and private hospitals. This makes awareness about CSP all the more important for Indian women and their families.
4. What Are the Symptoms?
This is where CSP becomes tricky. Many women with a scar pregnancy experience symptoms that could easily be mistaken for a normal early pregnancy or a routine miscarriage. Some women have no symptoms at all — which is why a first-trimester ultrasound is so crucial.
Light spotting or heavier bleeding in early pregnancy
A dull ache or cramping in the pelvic region
Many cases are detected only during a routine scan
With apparently normal early pregnancy signs
A sign of possible rupture — requires emergency care
Frequency or discomfort, depending on scar location
If you've had a previous C-section and experience any vaginal bleeding in early pregnancy — even light spotting — please see a doctor immediately. Do not wait to see if it "settles on its own."
5. How is it Diagnosed?
Diagnosis is primarily made through imaging — and the earlier it’s done, the better the outcome. At Vasundhara Hospital, we routinely recommend an early first-trimester ultrasound for all women with a prior cesarean scar.
Transvaginal Ultrasound (TVS)
This is the first and most important tool. A transvaginal scan gives a close, detailed view of the uterus and can identify a gestational sac implanted in the lower uterine segment, at or near the scar, rather than the uterine cavity.
Serum Beta-hCG levels
Blood tests to measure pregnancy hormone levels help track whether the pregnancy is growing normally or abnormally. In CSP, hCG levels may be elevated but inconsistent with normal growth.
Color Doppler Imaging
This specialized ultrasound measures blood flow to the gestational sac. In CSP, there is typically rich, high-velocity blood flow around the sac — a distinctive fingerprint that differentiates it from other conditions.
MRI (when needed)
For complex cases or when ultrasound results are unclear, an MRI provides a more detailed picture of the scar, the gestational sac, and surrounding tissue — helping surgeons plan the most appropriate treatment.
3D Ultrasound
In some advanced centers, 3D ultrasound helps create a volumetric view of the uterus to better assess scar thickness and the relationship of the sac to the bladder.
"The single most important thing you can do after a C-section is attend your early pregnancy scans without delay. A scar pregnancy caught at 6 weeks is a very different situation from one discovered at 10 weeks."
6. Types of Cesarean Scar Pregnancy
Not all scar pregnancies behave the same way. Researchers and clinicians have classified CSP into two main types based on how the pregnancy is implanting and growing — and this classification significantly affects the treatment approach.
Type 1 — Endogenic (Growing towards the uterine cavity)
In this type, the sac is implanted in the scar but is oriented towards the inside of the uterus. There may be some possibility of the pregnancy continuing, though it remains very high-risk. The uterine wall beneath the sac has some residual myometrium.
Type 2 — Exogenic (Growing towards the bladder)
Far more dangerous. Here, the sac implants deeply into the scar and grows outward, towards the bladder and abdominal wall. The overlying myometrium is very thin or absent. This type carries an extreme risk of uterine rupture and massive hemorrhage.
Type 2 CSP requires urgent treatment. The thinner the myometrial layer between the sac and the bladder, the higher the risk of catastrophic complications. This measurement — often 2–3mm or less — guides treatment urgency.
7. Treatment Options
There is no single “best” treatment for CSP. The right approach depends on gestational age, type of CSP, thickness of the remaining uterine wall, beta-hCG levels, patient’s desire for future fertility, and the expertise available at the treating hospital. Here is a breakdown:
| TREATMENT | HOW IT WORKS | BEST FOR | FERTILITY IMPACT |
|---|---|---|---|
| Methotrexate (MTX) | Injection that stops cell growth in the embryo, causing the pregnancy to resolve | Early diagnosis, low hCG, hemodynamically stable | Preserved |
| Uterine Artery Embolization (UAE) | Cuts blood supply to the sac; often combined with MTX or surgery | Rich blood supply to sac, high bleed risk | Usually preserved |
| Suction curettage | Surgical aspiration of the pregnancy under careful guidance | Selected early cases, after MTX | Preserved |
| Hysteroscopic resection | Minimally invasive removal of gestational tissue using a camera | Type 1 CSP, experienced operator | Preserved |
| Laparoscopic or open surgery | Removal of the sac and repair of the scar defect | Type 2 CSP, thick sac, failed MTX | Varies |
| Hysterectomy | Removal of the uterus | Life-threatening hemorrhage, family complete | Not preserved |
In most cases today, the goal is to treat the CSP while preserving the uterus and future fertility. Hysterectomy is reserved for emergencies when all else fails — and with good early diagnosis, it is rarely necessary.
With prompt diagnosis and modern minimally invasive techniques, the vast majority of women treated for CSP go on to recover well, retain their uterus, and have successful future pregnancies.
8. Risks If Left Untreated
CSP is not a condition that “goes away on its own.” Without treatment, the pregnancy continues to grow in tissue that cannot support it. As the weeks pass, the risks escalate rapidly.
-
Uterine rupture — The scar tissue tears under the pressure of the growing pregnancy, causing internal bleeding that can be life-threatening within minutes
-
Massive hemorrhage — Even without full rupture, the deeply invasive placenta can cause catastrophic blood loss during removal
-
Placenta accreta spectrum — CSP is closely related to placenta accreta, where the placenta invades deeply into or through the uterine wall
-
Bladder injury — Since the scar is near the bladder, invasion into surrounding structures is a serious risk
-
Loss of fertility — Emergency hysterectomy may be required if rupture occurs
-
Maternal death — In very advanced, undetected cases, CSP carries a real mortality risk
These risks are not meant to frighten you — they are meant to underscore one simple truth: early detection saves lives and saves uteruses.
9. Can I Have a Healthy Pregnancy After CSP?
This is the question we hear most often from our patients at Vasundhara Hospital — and the answer, in most cases, is yes.
Women who are treated early for CSP, especially with methods that preserve the uterus and repair the scar defect, have gone on to conceive again and deliver healthy babies. However, this comes with important caveats that your gynecologist will discuss with you in detail.
What to expect after CSP treatment
- A waiting period of at least 12–18 months before attempting conception again is generally recommended to allow the uterus to fully heal
- Any subsequent pregnancy will be considered high-risk and will require careful monitoring from the first trimester
- A repeat cesarean will likely be recommended, and the timing of delivery will be planned carefully
- The risk of recurrent CSP in future pregnancies exists, though it is not certain — early scanning becomes even more critical
- If the scar defect (niche) was surgically repaired during CSP treatment, the uterus may actually be structurally stronger for future pregnancies
Every woman’s situation is different. Some may be advised against further pregnancies depending on how the uterus has been affected. A thorough post-treatment evaluation and honest conversation with your doctor will give you the most accurate picture.
10. Prevention and Planning for the Future
Prevention of CSP begins even before a subsequent pregnancy. Here is what women with a previous C-section should know:
After your C-section
Ask your obstetrician about the condition of your scar. Some women have what’s called a “niche” — a small defect or indentation in the healed scar. If a significant niche is identified during a scan, it may warrant monitoring or even surgical repair before the next pregnancy.
Before the next pregnancy
Ideally, wait at least 18 months to 2 years after a C-section before trying to conceive. This gives the scar adequate time to heal. A pre-conception ultrasound to assess scar integrity is a good idea, especially if you’ve had multiple C-sections.
The moment you find out you’re pregnant
Register with an obstetrician immediately. Don’t wait until 12 weeks. An early transvaginal scan at 6–7 weeks of gestation is essential to confirm where the pregnancy has implanted. This is the most powerful preventive tool available.
Choosing the right hospital
If you have a previous C-section, ensure your antenatal care happens at a facility equipped to handle complications like CSP. This means access to high-resolution ultrasound, trained gynecologists, interventional radiology, and surgical expertise — all under one roof.
A Word from Vasundhara Hospital
We know that reading about something like Cesarean Scar Pregnancy can feel overwhelming — especially when you’re excited about a new pregnancy or planning for one. But at Vasundhara Hospital, we believe that an informed woman is an empowered woman.
Our team of experienced gynecologists and obstetricians is dedicated to walking alongside you through every stage of your reproductive journey. Whether you’re navigating a complicated diagnosis, recovering from CSP treatment, or simply planning your next pregnancy after a C-section — we are here, with the expertise and the compassion you deserve.
Get Expert Care at Vasundhara Hospital
Specialists in high-risk obstetrics, gynecologic surgery, and maternal–fetal medicine — here for you in Jodhpur.
Book a Consultation → vasundharahospital.comThis article is intended for general informational purposes and does not constitute medical advice. Every pregnancy and clinical situation is unique. Please consult a qualified medical professional for personalized guidance. © Vasundhara Hospital.